Febrile non-hemolytic transfusion reactions are the most common reaction reported after a transfusion. FNHTR is characterized by fever or chills in the absence of hemolysis (breakdown of red blood cells) occurring in the patient during or up to 4 hours after a transfusion.
What is the most common type of blood transfusion reaction?
According to the CDC , a febrile non-hemolytic transfusion reaction (FNHTR) is the most common reaction. It involves an unexplained rise in temperature during or 4 hours after the transfusion. The fever is part of the person’s white blood cells response to the new blood.
What is a febrile Nonhemolytic transfusion reaction?
Febrile nonhemolytic transfusion reactions (FNHTRs) are common, occurring with 1–3% of transfusions. FNHTR manifests as fever and/or chills without hemolysis occurring in the patient during or within 4 hours of transfusion cessation. Diagnosis is made by excluding other causes of fever.
What are the blood transfusion reaction?
The most common signs and symptoms include fever, chills, urticaria (hives), and itching. Some symptoms resolve with little or no treatment. However, respiratory distress, high fever, hypotension (low blood pressure), and red urine (hemoglobinuria) can indicate a more serious reaction.What is a ABO test?
The test to determine your blood group is called ABO typing. Your blood sample is mixed with antibodies against type A and B blood. Then, the sample is checked to see whether or not the blood cells stick together. If blood cells stick together, it means the blood reacted with one of the antibodies.
Which of the following is a potential acute transfusion reaction?
The most common immediate adverse reactions to transfusion are fever, chills and urticaria.
What is a haemolytic reaction?
A hemolytic transfusion reaction is a serious complication that can occur after a blood transfusion. The reaction occurs when the red blood cells that were given during the transfusion are destroyed by the person’s immune system. When red blood cells are destroyed, the process is called hemolysis.
What is Taco transfusion reaction?
Transfusion-associated circulatory overload (TACO) is a common transfusion reaction in which pulmonary edema develops primarily due to volume excess or circulatory overload.What is ABO incompatibility reaction?
ABO incompatibility happens when a mother’s blood type is O, and her baby’s blood type is A or B. The mother’s immune system may react and make antibodies against her baby’s red blood cells. The consequences and treatment are similar to Rhesus disease. Check Jaundice in babies.
What is non haemolytic reaction?Hematology. Febrile non-hemolytic transfusion reaction (FNHTR) is the most common type of transfusion reaction. It is a benign occurrence with symptoms that include fever but not directly related with hemolysis.
Article first time published onWhat does Nonhemolytic mean?
Definition of nonhemolytic medical. : not causing or characterized by hemolysis : not hemolytic a nonhemolytic streptococcus.
What is ABO Rh O positive?
Possible ABO blood groups include O, A, B, or AB. The Rh antigen is another compound that may or may not be present on the surface of red blood cells. The Rh test determines whether this configuration is present (“Rh-positive”) or absent (“Rh-negative”) on an individual’s blood cells.
What does Rhesus D positive mean?
If you’re rhesus positive (RhD positive), it means that a protein (D antigen) is found on the surface of your red blood cells. Most people are RhD positive. If you’re rhesus negative (RhD negative), you do not have the D antigen on your blood cells.
Which ABO blood type is least common?
However, in the United States, AB-negative is considered the rarest blood type, and O-positive is the most common. The Stanford School of Medicine Blood Center ranks blood types in the United States from rarest to most common as follows: AB-negative (.
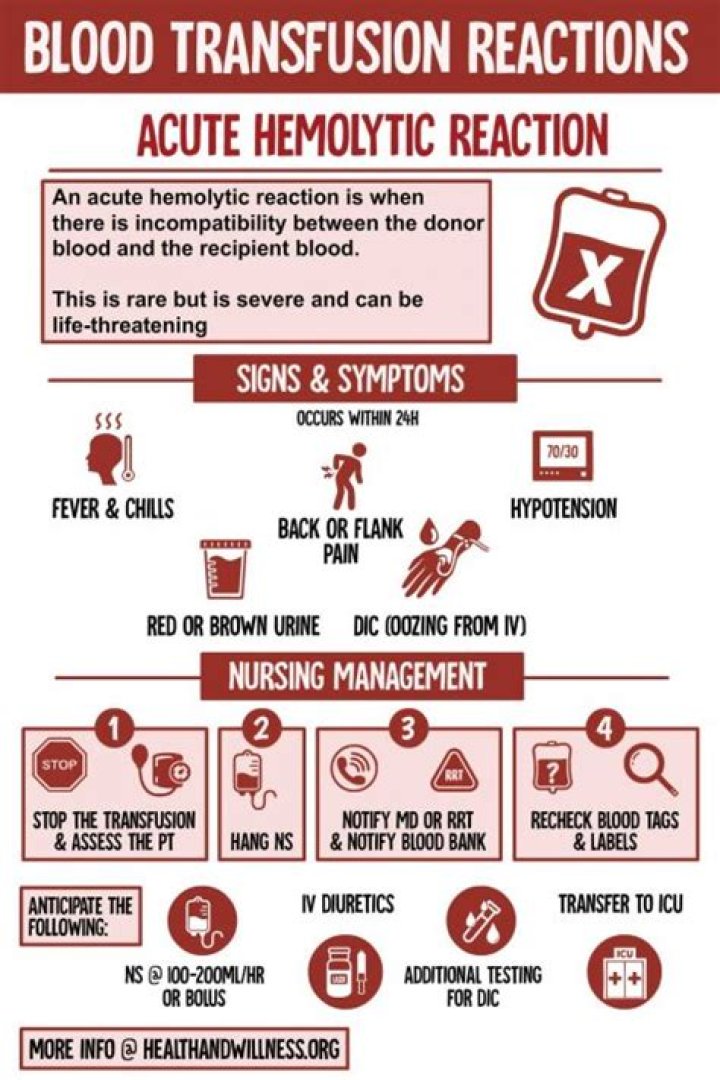
What is the most common cause of an acute hemolytic transfusion reaction?
Acute hemolytic transfusion reactions are usually caused by ABO incompatibility. This potentially fatal complication occurs in about 1 in 30,000 transfusions. As little as 20 to 30 mL of incompatible RBCs can cause agitation, nausea and vomiting, dyspnea, fever, flushing, hypotension, tachycardia, and hemoglobinuria.
What is post transfusion purpura?
Post-transfusion purpura (PTP) is a rare yet serious disease characterized by severe thrombocytopenia occurring after a blood transfusion. It is caused by alloimmunization against platelet antigens, anti-HPA-1a being the most frequent antibody.
What is the meaning of alloimmunization?
Alloimmunization is defined as an immune response to foreign antigens after exposure to genetically different cells or tissues. Although alloimmunization is a natural event during pregnancy, frequently it is the undesirable outcome of a blood transfusionand/or transplant.
What is an immediate immunologic transfusion reaction?
Among the immediate complications of transfusion, the most common and serious are intravascular hemolytic transfusion reactions because of ABO incompatibility caused by giving the wrong blood to a patient (e.g. group A blood to a group O recipient).
Is hypertension a blood transfusion reaction?
Infective shock. Bacterial contamination of a blood component is a rare but severe and sometimes fatal cause of transfusion reactions. Acute onset of hypertension or hypotension, rigors and collapse rapidly follows the transfusion.
When does hemolytic transfusion reaction occur?
Acute hemolytic reactions happen within 24 hours of transfusion and delayed hemolytic reactions happen after 24 hours. Delayed reactions usually occur two weeks after but can go up to 30 days post transfusion.
How common is ABO incompatibility?
ABO incompatibility in the newborn generally presents as neonatal jaundice due to a Coombs positive hemolytic anemia and occurs in 0.5-1% of newborns.
What is the difference between Rh incompatibility and ABO incompatibility?
ABO incompatibility is less severe than Rh incompatibility because there are fewer group A or B antigen sites on neonatal red blood cells compared with Rh antigens, allowing sensitized A or B cells to survive longer in the infant’s circulation than with anti-Rh antibodies.
Is positive and O positive compatible?
Type O positive blood is given to patients more than any other blood type, which is why it’s considered the most needed blood type. … O positive red blood cells are not universally compatible to all types, but they are compatible to any red blood cells that are positive (A+, B+, O+, AB+).
What transfusion reaction is similar to TACO?
Circulatory overload from fluid infusion (including blood transfusion) is common in elderly patients and patients with heart failure and managed along similar lines—TACO is seen as a complication of fluid infusion rather than blood transfusion.
How common is Trali?
TRALI has been reported following transfusion of all plasma-containing blood components. Estimates of the incidence of TRALI have been 1 in 5,000 components, mostly in whole blood (1), 1 in 7,900 units of fresh frozen plasma (51), and 1 in 432 units of whole blood-derived platelet concentrates (13).
What is the difference between Trali and TACO?
Diagnostically, it remains very challenging to distinguish TACO and TRALI from underlying causes of lung injury and/or fluid overload as well as from each other. TACO is characterized by pulmonary hydrostatic (cardiogenic) edema, whereas TRALI presents as pulmonary permeability edema (noncardiogenic).
What are three clinical manifestations of circulatory overload?
Signs and symptoms include dyspnea, orthopnea, wheezing, tightness in the chest, cough, cyanosis, tachypnea, rapid increase in blood pressure, distended neck veins, and S3 on auscultation. Peripheral and pulmonary edema may also develop.
Why does circulatory overload occur?
Circulatory (volume) overload occurs when the volume of the transfused blood components and that of any coincidental infusions cause acute hypervolemia. Typically, this causes acute pulmonary edema.
What causes febrile reaction?
Most febrile reactions that occur during transfusion of red blood cells are caused by the interaction of leukocyte antibodies in the recipient’s plasma with donor leukocytes, stimulating the release of pro-inflammatory cytokines such as interleukin-1 (IL-1), interleukin-6 (IL-6) and tumor necrosis factor alpha (TNF).
What does alpha haemolytic mean?
Alpha hemolysis (α) is the reduction of the red blood cell hemoglobin to methemoglobin in the medium surrounding the colony. This causes a green or brown discoloration in the medium. The color can be equated with “bruising” the cells.
What is the difference between alpha and beta hemolysis?
Alpha Hemolysis is the process of incomplete destruction of red blood cells in the blood. Beta Hemolysis is the process of complete destruction of red blood cells in the blood. In alpha hemolysis, red blood cells break down completely. In beta hemolysis, red blood cells break down partially.