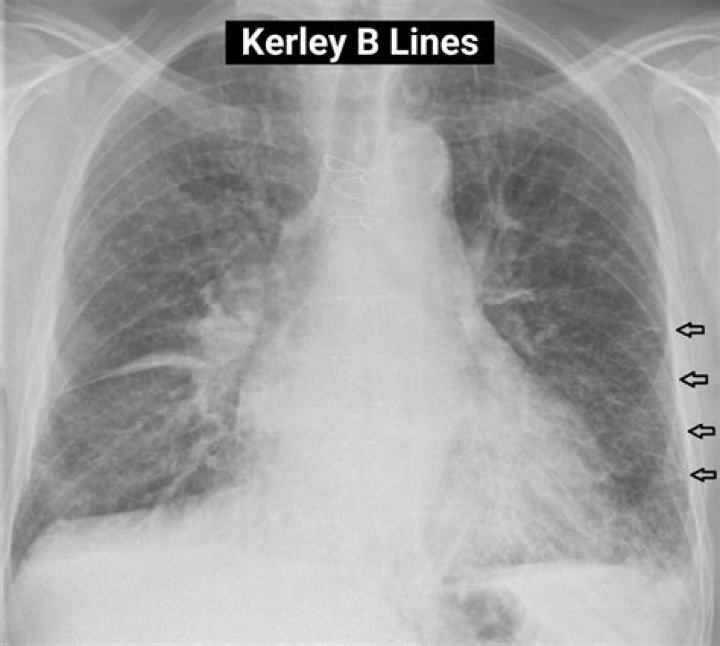
Kerley B lines are small, horizontal, peripheral straight lines demonstrated at the lung bases that represent thickened interlobular septa on CXR. They represent edema of the interlobular septa and though not specific, they frequently imply left ventricular failure.
What are B lines on ultrasound?
B lines, previously termed ”comet tails,” are vertical hyperechoic reverberations moving synchronously with the lung and represent key artifacts in interpreting pulmonary ultrasound findings [3,4]. The physiologic basis of B lines relates to decreased lung aeration [5], a finding that is nonspecific.
What do Kerley B lines look like?
Kerley B lines These are thin lines 1-2 cm in length in the periphery of the lung(s). They are perpendicular to the pleural surface and extend out to it. They represent thickened subpleural interlobular septa and are usually seen at the lung bases.
What causes B lines on ultrasound?
In the presence of extravascular lung water (EVLW), the ultrasound beam finds subpleural interlobular septa thickened by edema. The reflection of the beam creates some comet-tail reverberation artifacts, called B-lines or ultrasound lung comets.What is septal line thickening?
Diffuse interlobular septal thickening (DIST) is a pattern of lung disease found on high-resolution thoracic CT scanning (HRCT or CTPA). It represents pathology in the periphery of the pulmonary lobules (ie, the interlobular septa).
Can ultrasound see lungs?
It uses sound waves to look at the structures and organs in your chest. It can help your healthcare provider see how well your lungs and heart are working. A chest ultrasound can look at these areas: Lungs.
What is Kerley C lines?
Kerley C lines. These are the least commonly seen of the Kerley lines. They are short, fine lines throughout the lungs, with a reticular appearance. They may represent thickening of anastomotic lymphatics or superimposition of many Kerley B lines.
What does lung sliding mean?
Lung sliding has been described as a shimmering appearance of the pleura, or like tiny ants marching on a string. The pleura will seem to slide back and forth as the patient breathes. Comet tails, vertical artifacts originating from the pleura, may be visible on ultrasound, also proving the lung is inflated (Figure 2).What is lung sliding?
Lung sliding is the respirophasic shimmering to and fro movement of the visceral and parietal pleural surface. The presence of lung sliding indicates that the lung is fully inflated at the site of probe placement on the chest wall, so there is no pneumothorax at that examination site.
What do B lines mean?The B-line is a kind of comet-tail artifact indicating subpleural interstitial edema. The relationship between anterior interstitial edema detected by lung ultrasound and the pulmonary artery occlusion pressure (PAOP) value was investigated.
Article first time published onAre B lines normal?
A few B-lines (<3/field of view) can often be found under normal circumstances, especially in the elderly, and around the base of the lungs 4.
What is lung pulse?
Lung pulse is the cardiophasic movement of the visceral parietal pleural surface (arrow). The presence of lung pulse indicates that the lung is fully inflated at the site of probe placement on the chest wall, so there is no pneumothorax at that examination site.
What is Hampton hump?
Hampton’s hump is a radiological sign consisting of a peripheral, wedge-shaped opacification adjacent to the pleural surface, which represents pulmonary infarction distal to a pulmonary embolus. 1. Owing to good pulmonary perfusion from collateral blood vessels, this sign is rarely seen in clinical practice.
What swollen lungs?
Pulmonary edema is a condition caused by excess fluid in the lungs. This fluid collects in the numerous air sacs in the lungs, making it difficult to breathe. In most cases, heart problems cause pulmonary edema.
What is a phantom tumor?
— The “phantom tumor” is a roentgenographic finding caused by fluid localizing in an interlobar fissure of the lung secondary to congestive heart failure. These fluid accumulations have also been called “vanishing tumor” and “pseudo tumor” of the lung because they tend to disappear when the heart failure is treated.
What are septa in lungs?
These septa are composed of connective tissues within which run the pulmonary veins and lymphatics which drain towards the pleura. … The interlobular septa are incomplete allowing for communication between adjacent secondary pulmonary lobules (canals of Lambert and pores of Kohn).
What is the most common cause of interstitial lung disease?
A bacteria called Mycoplasma pneumoniae is the most common cause. Idiopathic pulmonary fibrosis. This makes scar tissue grow in the interstitium.
What is Cephalization on chest xray?
Cephalization refers to the redistribution of blood into the upper lobe vessels. It has been hypothesized that once the hydrostatic pressure exceeds 10 mm Hg, then fluid begins to leak into the interstitium of the lung.
Where are Kerley B lines found?
Linear Patterns Kerley’s B lines, which reflect thickening of the subpleural interstitial compartment, typically are about 1 cm in length and 1 mm in thickness and usually found in the periphery of the lower lobes, abutting the pleura.
What Orthopnea means?
Orthopnea is the sensation of breathlessness in the recumbent position, relieved by sitting or standing. Paroxysmal nocturnal dyspnea (PND) is a sensation of shortness of breath that awakens the patient, often after 1 or 2 hours of sleep, and is usually relieved in the upright position.
What is upper lobe blood diversion?
Upper lobe pulmonary venous diversion (also described as cephalisation of the pulmonary veins) reflects elevation of left atrial pressure and is an early sign of pulmonary oedema.
How do you know if there's something wrong with your lungs?
- Trouble breathing.
- Shortness of breath.
- Feeling like you’re not getting enough air.
- Decreased ability to exercise.
- A cough that won’t go away.
- Coughing up blood or mucus.
- Pain or discomfort when breathing in or out.
What shows up on a chest xray?
Chest X-rays produce images of your heart, lungs, blood vessels, airways, and the bones of your chest and spine. Chest X-rays can also reveal fluid in or around your lungs or air surrounding a lung.
Why is ultrasound not used for lungs?
The concept that ultrasound cannot be employed for evaluating the lung is linked to the presence of air, which determines a high acoustic mismatch with the surrounding tissues, causing a complete reflection of the ultrasound beam, preventing the creation of direct imaging of the pulmonary parenchyma [2].
What is the M mode?
M-mode is defined as time motion display of the ultrasound wave along a chosen ultrasound line. It provides a monodimensional view of the heart. All of the reflectors along this line are displayed along the time axis.
What is a positive FAST exam?
FAST is most useful in trauma patients who are hemodynamically unstable. A positive FAST result is defined as the appearance of a dark (“anechoic”) strip in the dependent areas of the peritoneum. In the right upper quadrant this typically appears in Morison’s Pouch (between the liver and kidney).
What does a pneumothorax look like on xray?
Finding of pneumothorax on chest radiographs may include the following: A linear shadow of visceral pleura with lack of lung markings peripheral to the shadow may be observed, indicating collapsed lung. An ipsilateral lung edge may be seen parallel to the chest wall.
What is a Hydropneumothorax?
Hydropneumothorax is the abnormal presence of air and fluid in the pleural space. The knowledge of hydropneumothorax dates back to the days of ancient Greece when the Hippocratic succussion used to be performed for the diagnosis.
Why is pleurodesis performed?
Pleurodesis is a procedure performed to obliterate the pleural space to prevent recurrent pleural effusion or pneumothorax or to treat a persistent pneumothorax.
Do a lines rule out pneumothorax?
Sonographic signs, including ‘lung sliding’, ‘B-lines’ or ‘comet tail artifacts’, ‘A-lines’, and ‘the lung point sign’ can help in the diagnosis of a pneumothorax. Ultrasound has a higher sensitivity than the traditional upright anteroposterior chest radiography (CXR) for the detection of a pneumothorax.
What are Z lines on lung ultrasound?
Z lines are vertical, bundle-like shaped lines arising from the pleural line; however, they are ill-defined, do not erase A lines and are not perfectly synchronous with respiratory movements.